Overcoming Onychomycosis™ By Scott Davis If you want a natural and proven solution for onychomycosis, you should not look beyond Overcoming Onychomycosis. It is easy to follow and safe as well. You will not have to take drugs and chemicals. Yes, you will have to choose healthy foods to treat your nail fungus. You can notice the difference within a few days. Gradually, your nails will look and feel different. Also, you will not experience the same condition again!
What is the prevalence of insomnia in postnatal women, and how do infant-sleep-alignment strategies compare with parental counseling?
The prevalence of insomnia in postnatal women is remarkably high, with studies indicating that while over 80% experience significant sleep disturbances, between 10% and 30% meet the clinical criteria for an insomnia disorder, a rate substantially higher than in the general female population. When managing this issue, infant-sleep-alignment strategies, which focus on modifying the baby’s sleep patterns to indirectly benefit the mother, are often less effective for treating maternal insomnia than parental counseling, particularly Cognitive Behavioral Therapy for Insomnia (CBT-I), which directly addresses the mother’s own maladaptive sleep behaviors and anxieties.
😴 The Widespread Challenge of Postnatal Insomnia
The transition to motherhood is a period of profound physiological and psychological change, and for a vast number of new mothers, it is accompanied by a significant disruption to sleep. The prevalence of postnatal insomnia is a major public health concern, though figures can vary based on the specific definitions and assessment methods used. Broadly, studies report that up to 80% of women in the first few months postpartum experience severe sleep fragmentation and poor sleep quality, largely due to the demands of a newborn.
However, experiencing poor sleep is different from having a clinical insomnia disorder. Postnatal insomnia, as a clinical condition, involves difficulty falling asleep, staying asleep, or waking too early, despite having the opportunity to sleep, leading to significant daytime distress and impairment. When using strict diagnostic criteria, systematic reviews and large-scale studies estimate that the prevalence of clinical insomnia disorder in the postnatal period ranges from 10% to 30%. This rate is approximately two to three times higher than that observed in the general population of women of the same age. The highest rates are often seen in the first three to six months after birth, a time when infant sleep is at its most unpredictable. This condition is not merely a transient phase of “new parent tiredness”; it is a distinct disorder with significant consequences, including an increased risk for postpartum depression, anxiety, and impaired mother-infant bonding.
👶 Infant-Sleep-Alignment Strategies: An Indirect Approach
A common and intuitive approach to improving maternal sleep is to focus on the primary source of the disruption: the infant. Infant-sleep-alignment strategies encompass a range of behavioral interventions designed to help the baby consolidate their sleep, sleep for longer stretches, and learn to self-soothe. The underlying theory is simple: if the baby sleeps better, the mother will get more opportunities for uninterrupted sleep.
These strategies include several popular methods:
- Graduated Extinction: Often referred to as the “Ferber method,” this involves letting the infant cry for progressively longer intervals before offering brief comfort, teaching them to fall asleep independently.
- Bedtime Fading: This technique involves temporarily putting the baby to bed later, closer to when they naturally fall asleep, and then gradually moving the bedtime earlier.
- Routine Establishment: This focuses on creating a predictable and calming bedtime routine (e.g., bath, book, song) to signal to the baby that it is time for sleep.
While many studies show that these interventions can be effective in improving infant sleepleading to fewer night wakings and longer sleep durations for the babytheir impact on maternal insomnia is less direct and more variable. For mothers whose sleep problems are solely a result of being woken by their infant, these strategies can provide significant relief. By reducing the number of night-time awakenings, the mother gains more consolidated sleep. However, for a woman with a true insomnia disorder, this approach often falls short. Her inability to sleep may persist even when the baby is quiet. She might lie awake for hours after a feeding, her mind racing with anxiety, or find she cannot fall back asleep after being woken, a condition known as sleep-maintenance insomnia. Therefore, while beneficial for the infant and helpful for maternal sleep opportunity, these strategies do not address the mother’s own physiological and psychological barriers to sleep
🧠 Parental Counseling: A Direct Treatment for Maternal Insomnia
In contrast to infant-focused methods, parental counseling directly targets the mother’s own sleep patterns, thoughts, and behaviors. The most evidence-based and effective form of this counseling is Cognitive Behavioral Therapy for Insomnia (CBT-I). CBT-I is a multi-component therapy that addresses the root causes of insomnia and is now considered the first-line treatment for the disorder.
CBT-I for postnatal women is adapted to their unique circumstances and typically includes:
- Sleep Restriction: This component involves limiting the time spent in bed to more closely match the actual amount of time the mother is sleeping. This mild sleep deprivation helps to consolidate sleep and increase the natural drive to sleep, making sleep more efficient.
- Stimulus Control: This re-establishes the bed as a cue for sleep. It involves strict rules, such as only using the bed for sleep and intimacy, and leaving the bedroom if unable to fall asleep within about 20 minutes. This breaks the frustrating cycle of lying in bed awake.
- Cognitive Restructuring: This is the “cognitive” part of the therapy. It helps the mother identify and challenge anxious thoughts and unrealistic beliefs about sleep (e.g., “If I don’t get eight hours of sleep, I will be a terrible mother tomorrow”). By reframing these thoughts, it reduces the anxiety and mental arousal that prevent sleep.
- Relaxation Techniques: Mothers are taught techniques like diaphragmatic breathing, progressive muscle relaxation, or guided imagery to calm the mind and body before sleep.
⚖️ Comparing the Two Approaches: Indirect vs. Direct Intervention
The comparison between infant-sleep-alignment strategies and parental counseling reveals a fundamental difference in their targets and mechanisms. Infant-focused strategies are an indirect environmental intervention. They aim to create a quieter environment with more opportunities for sleep. Their success is contingent on the mother’s ability to capitalize on these quiet periods. If the mother’s insomnia is characterized by hyperarousal and anxiety, a sleeping baby in the next room does not guarantee her own sleep.
Parental counseling, specifically CBT-I, is a direct psychophysiological intervention. It targets the mother’s internal stateher sleep drive, her anxious thoughts, her conditioned arousal to the bedroom. Clinical trials have shown that CBT-I is highly effective for treating postnatal insomnia, often leading to significant and lasting improvements in sleep quality, reduced nighttime wakefulness, and decreased daytime fatigue. It empowers the mother with lifelong skills to manage her own sleep.
In an ideal care model, the two approaches are not mutually exclusive but can be complementary. Establishing healthy sleep habits for the infant is a valuable goal for the entire family. However, when a mother is suffering from a clinical insomnia disorder, simply fixing the baby’s sleep is an incomplete and often insufficient solution. Direct parental counseling that addresses her specific sleep-related anxieties and behaviors is essential for her recovery and overall well-being.
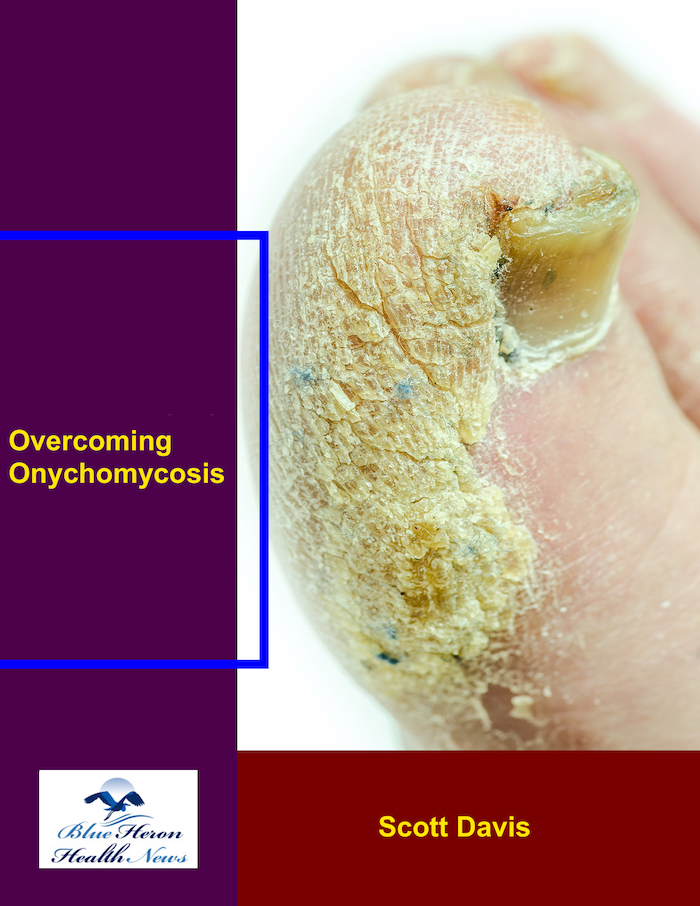
Overcoming Onychomycosis™ By Scott Davis If you want a natural and proven solution for onychomycosis, you should not look beyond Overcoming Onychomycosis. It is easy to follow and safe as well. You will not have to take drugs and chemicals. Yes, you will have to choose healthy foods to treat your nail fungus. You can notice the difference within a few days. Gradually, your nails will look and feel different. Also, you will not experience the same condition again!

I’m Mr.Hotsia, sharing 30 years of travel experiences with readers worldwide. This review is based on my personal journey and what I’ve learned along the way. Learn more |
